A version of this post has been published on Medium.
Prologue

Marc is a
Principal at Fit Associates, a firm based in Pittsburgh, PA that helps people
learn to create change together; he also teaches at CMU and SVA DSI. I met Marc many years ago when he was Chief
Experience Officer at a Chicago-based design firm called HannaHodge. (Marc,
always a trail blazer, was the first Chief Experience Officer anywhere ever.)
In April, I interviewed Marc when he met with my students remotely during a
course I was teaching at the Austin Center for Design. I invited Marc to extend
that conversation.
---
Posing the big question, and seeing companies as emergent patterns of relationship
Richard: I’ve been exploring what it takes for companies to become (more)
“ethical” — to pursue goals that are, for example, social or environmental as
vigorously as goals that are economic — to move beyond side Corporate Social
Responsibility initiatives that many claim exist mostly for PR reasons or to
make employees happier about working there. Jon Kolko and I addressed this a
bit in our conversation on the relationship between design and activism,
and you began to address it in February via a Twitter conversation you had with Jared Spool.
Do you have the
answer? Do you know what it takes for companies to (begin to) make it (more of)
their responsibility to improve society or the environment?
Gardening versus changing
Marc: Hoo boy, there’s a lot in there.
I’m not saying
this is what you asked for, but a question like that can seem to expect a
direct, action-oriented answer: “The Thurston-McKinney approach will set you on
the right path for sure.”
But of course
it’s messier than that. There ARE some good ways to get started, and good tools
we can bring to bear. But that beginning and those tools are systemic rather
than direct.
So I need to
start with a way of seeing organizations and change that’s different than the
view we all seem to have soaked up through the Big Old Societal Story.
A company is an
emergent system made of people in loose relationship, not a machine made of
parts in tightly constrained order. We can’t “work on it” with predictable
results.
It is more
accurate and useful to see an organization as a process. And to notice that
this process (or really this woven bundle of patterns of processes) is mostly concerned
with reinforcing its existing structures and repeating its old processes and
stories. That process view of organizations gives us…
--Useful question #1--
How can we
nurture the conditions in which at least some part of the organization pauses
its process of repetition and reinforcement of the old story, so it can begin
exploring a new story?
As some systems
sage has pointed out, “No gardener ever made a rose.” But good gardeners are
great at working with the conditions in which roses can become healthy and flourishing. That is a clue.
Relationships as our "material"
I’ll make one
more point about social systems, then I’ll pause.
Say you’re
setting out to influence or change an organization to “take responsibility to
improve society and the environment.” The most common thing has been to focus
on the people—the executives and managers maybe, or the strategic innovation
group. The naïve idea is to somehow persuade or motivate them to care, to take new
actions, to measure success by different values. This kind of persuasion has
been tried so many times in so many ways, we can say confidently that
persuasion is a dull tool.
If people are the
“material” of our approach to change, then we’ve got two problems. One is that we’re
working with the least malleable aspect of the system. All the models of
individual change tell us that it takes time, it’s not easy, and it doesn’t happen
because someone else wants it to.
The other problem
is that we’re trying to apply a parts-and-whole view of a system, when social
systems are mostly made of relationships. It’s easy to see the outcomes we’d
like to change as coming from the people in the organization. But that’s not
what’s really going on. The outcomes emerge
from the relationships between those people, and from thousands and thousands
of conversations across those relationships. For the topic we’re discussing,
there’s barely even such a thing as an individual person.
When we focus on
relationships as our “material,” we see people as participants. We become
interested in the conversations through which those relationships are formed
and maintained or blocked and disrupted. We notice how a large proportion of
those conversations have to do with maintaining and repeating the status quo.
“Johnson, I know you’re new here and full of ideas, but why can’t you be more
like Williams? He was innovator of the year!”
Conversations
shape relationships, relationships play a dominant role in individual change
and development, and conversations are far more malleable than individual human
behavior. So if people are not the “material” of change, but instead we’re
focused on patterns of conversation and relationship, we have,
--Useful question #2--
How can we work with conversation and
relationship in ways that can attract and sustain new patterns of
organizational behavior?
Organizational narratives, the seeds of change, and four ways to "cross the gap"
Richard: Great questions, both prompting additional questions.
Regarding the
first… I don’t want to over-extend the metaphor, but don’t good gardeners ever
plant the seeds in addition to working the conditions in which the roses become
healthy and flourish? Or, within an organization, is it better to find the
desirable seeds that have already been planted or just assume they are there
somewhere? If one of the latter, how does one gain access to nurture their
growth (or must all change occur from within)?
And both of your
questions bring to mind John Hagel’s concept of a “narrative” which, unlike a “story” which, as defined by Hagel, has a beginning, middle,
and end, is open-ended, inviting participation and contribution to shape how it
unfolds. According to Hagel’s definition, a corporate narrative is about the
corporation’s audience rather than about itself. Nevertheless, how can a
narrative about the goals and roles of a company become a part of the
conversations its people have and, hence, the relationships those conversations
help shape? And how can such conversations and new relationships be nurtured?
However, isn’t
the approval of people still needed? Don’t people still need to be convinced at
some point or at multiple points that change — even change in the form of
different conversations — is beneficial? While facilitating the exploration of
a new corporate story via nurturing new conversations is important, people
still need to be persuaded.
Marc: I like your question about where
the seeds come from. Sometimes I use a little drawing to talk about that
question. On the left side is “the way things are,” on the right is “the way
things could be” or the way we’d like them to be, or sense that it is possible
to be. And in between is a gap.
Somebody, it might be Brené Brown, calls that “the
cynicism gap.” It’s the gap we aren’t sure how to cross, and with enough
repeated disappointment we might start to believe it can never be crossed.
Water the sprouts that already exist
So how do we work? How do we go about getting ourselves
across the gap together? One answer is to look for the seeds that already
exist. John Thackara sometimes says, “What needs to
happen is already happening.” By which he means, whatever big challenge or
stuck situation you’re considering, you’re almost certainly not the only one.
Others have already started, some have made progress, and a couple of them are
probably onto something.
Then he says, “You just need to find where it’s
happening, connect those people to each other, and ask them what they need to
grow.” And he’s more or less made a career out of that statement.
Plant new seeds
So that’s the approach of “The seeds have already been
planted.” And you’re right, there’s also the “Let’s plant some seeds ourselves”
approach. We can manage a portfolio of little pop-up futures—experiments to
find out what will attract people toward new patterns of behavior and
relationship. I draw them like this, like they’re able to latch on to the edge
of the gap and pull it closed.
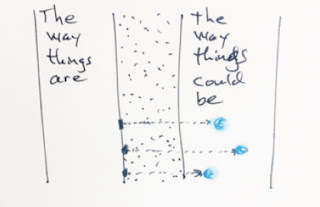
These aren’t prototypes in the way the business and
design world usually thinks of them. They are experiences of a possible way of
living, working, relating, etc. For example, “You’ve said your two departments
don’t get along and seldom talk. Each of you send a vertical cross-section of
your people, and for one week you’ll try three different kinds of collaboration
and communication. At the end of the week you’ll design a set of
inter-department experiments—artifacts, roles, rituals, practices, processes,
etc.—that a) you have reason to believe might work, b) you can establish as
practice if they’re great, and c) you can stop if they’re not great without
causing any damage.
There are at least two other overall strategies for
crossing the gap. I’ll say less about them, but just to complete the list, one
is to build creative capacity in the community so more seeds will sprout on
this side of the gap. Another is to convene across the system and make a
facilitated journey of co-creation together. These all have different expressions
in different fields, but so far as I’ve been able to find those are four ways
people are successfully going about crossing the gap.
Both of those “seed” approaches—planting seeds and nurturing
the sprouts you find—are grounded in good theory about how socially complex
systems change. You don’t shift the dominant paradigm through direct pressure
on its center. You don’t persuade those who are fully invested in the old
pattern, convincing them to change their minds and adopt a new one. Instead of
persuading, you attract to something. You activate urges that are already present.
Some people call the experiments and sprouts “hopeful monsters.” To people in the comfortable middle
of the system, they’re strange. They look like monsters. But to others they are
hopeful, they are attractive. As they become more visible, as they connect,
they become more and more ready to move to the center once it inevitably
weakens.
Persuasion vs. attraction and the stories that keep us stuck
That point about attraction versus persuasion connects to
your question about narrative. Narrative or story is a hugely important topic.
In our work with facilitation (“hosting conversations that matter”), we are
sometimes very deliberate in working with the kind of deep narrative you
describe.
I mentioned people who are fully invested in the old
pattern. They repeat and reinforce its behaviors and relationships. “Johnson,
you’re doing it wrong. Why can’t you be more like Williams?” What’s under that?
Where does it come from? It comes from that underlying narrative about the
company, its place in the world, and their place in it. It might be
unconscious. But it is repeated constantly in the choices of who to reward, who
to mock, what to prioritize, what to fight for and against.
“We sell as much coffee as we possibly can.”
“We provide the comforts of home and office, with
coffee.”
“We are partners with the planet and society in the use
of coffee.”
The old story is comfortable. We’ve been living it a long
time, we know how to do it, we know our role. But we have to stop the old story
in order to find the new one. It’s uncomfortable—a real stretch!—to hit pause
on the story that defines your identity and your place in it all, and move into
a place between stories—a place that makes room for uncertainty, that gives
time to find the new story that has the strength to draw you out into new
patterns.
You asked how this kind of conversation can be nurtured. And
you asked if it isn’t always the case that some people need to be persuaded to
change, to explore, to let go of the old story and consider a new one.
Can you persuade
someone to have an open mind? I find persuasion to be the dullest knife in the
drawer, but for reasons I don’t understand it’s the one people always seem to
reach for.
If you like I can expand and give examples, but the big picture
answer is to say, 1) experiences have far more power to open minds than any
argument, and 2) there is a very old craft of hosting conversations in
ways that make it more likely that people will suspend their presuppositions,
see through other people’s eyes, reflect and reframe together. And we can
connect those experiences over time with some real hope of shifting things.
Earlier in this conversation I mentioned that it’s useful
to view a company as a process, busily repeating its patterns or perhaps
experimenting with new ones. Exactly the same can be said of people. Of
leaders, decision-makers, designers, builders. They are in the process of
repeating their old stories, and/or becoming the next version of themselves.
The gardener suggests tending to the conditions for their becoming, rather than
trying to persuade them to stop being who they are.
What does that look like?
Richard: Suspending presuppositions, seeing through
other people’s eyes, reflecting and reframing with others, … — all skills
purportedly in the designers’ wheelhouse, and while perhaps those experiments
with other ways of doing things aren’t prototypes in the way the design world
usually thinks of prototypes, it seems like designers are at least somewhat
well-equipped (and are well-positioned to become better equipped) to play a key
role in making or helping to make all of this happen. But how might they be
empowered to do so? Via experiments with such empowerment?
Plus, since we’re
discussing all this in the context of exploring what it takes for companies to
(begin to) make it their responsibility to improve society or the environment,
what might little experiments in that
direction look like?
The indiscernible beginnings of a storm of change
Marc: Maybe it will help to try to make up a story – a bit of process
fiction. The story is needed because my response to the two things you just
asked about--the prototypes and the role of designers--need the context of a
bigger story.
How does the
story get started? What is the beginning of an organizational shift toward
social and environmental responsibility? In her book, The Storm of Creativity, Kyna Lesky wonderfully compares creativity
to a thunderstorm. When does a storm begin? What is the sequence that leads to
the formation of the right clouds, the right conditions? What reinforces those
conditions until the rain begins to fall? We can’t say, because it is not a
matter of direct cause and effect. It is a matter of pattern emergence in
complexity.
So in our
imaginary organization let’s say there are the seeds of a storm. There are
people who feel uneasy with the status quo. A few managers have been to the
Sustainable Brands conference. HR has hired a diversity and inclusion manager,
and emails are circulating about other companies’ local community efforts. This
is the visible, surface evidence – the smoke. The fire producing that smoke is
still invisible in the quarterly reports and project briefs. It’s still in the
form of coals, deep in people’s thoughts and emotions. Managers who find
themselves daydreaming on the drive home, wondering about moving to a company
where they can feel like they’re giving something to the world other than more
disposable containers.
It starts with listening
Should we make
this story about a lone catalyst? A team leader somewhere, not a VP or
anything, who decides to begin taking action? Or should we make this about
someone more senior who has a little budget and power to convene? Either way,
the first step is to listen.
What does it look
like when we listen to an organization? With a full dose of “it depends,”
listening might involve….
- Making a map of
leaders and influencers, and scheduling time for deep “dialogue interviews.” More
personal than business or research interviews: the story of how they got where
they are, what they really care about, what they’re trying to accomplish and
what’s in the way, the values that underlie their work, and whether they think
about their legacy—how things will be different because of their time at the
company.
- Something more
systematic like a culture scan, gathering stories about the way choices are
made, the way the organization is and isn’t already living out the sort of
policies and behaviors we’re aspiring to. The patterns in those stories suggest
where the “adjacent futures” might be—informal patterns and practices that some
people are already living, moving toward, and which others feel attracted to.
- Finding the
pioneers, asking what they need, and helping them connect to each other. It is
often (always?) the case that when a system or paradigm is peaking, is dominant
-- like the one playing out in our imaginary organization that’s driven by
concerns other than long-term quality of life for all species – that’s the time
when some folks become dissatisfied and start jumping off. They might not know
exactly what they’re jumping toward, but they can see how things can be better,
they see the damage of the status quo, and they head out to experiment. They
are the seeds of the next thing. Help them find each other!
In the case
studies we’ve looked at, people take up to a year to simply listen to the
system, gather people for conversation, sense what’s going on, and put in place
the conditions for the next steps to be perceived as legitimate.
Our beliefs about change affect our default approach
Where does it go
from there? I’m working on a piece of writing that describes how our world view
– the story we’ve chosen to believe about change – strongly affects the way we
think it’s “smart” to go about working toward change.
Do you believe we
can manage our way to just, equitable, and sustainable practices through an
innovation process? Do you believe shifting the system will require a
whole-system approach? Maybe you believe in bottom-up change and the power of
the grassroots, or the power of community and dialogue across boundaries. The
importance of building capacity for participation and co-creation? The power of
place?
My point is not
that there is confusion about approach, or that change strategies are purely subjective.
My point is that organizations are complex in a truly formal sense: emergent,
nonlinear, unpredictable. And we live and work in a time of great energy toward
finding better ways to engage with that kind of social complexity. Out of that
energy comes a lot of inadequate approaches—nice tries, no cigar. There is a
lot of “I’ll just keep swinging this same hammer at these things I’ve decided
to call nails.” And there are a few really beautiful hard-working approaches we
can learn from. They all originated outside the “design” conversation. One or
two are starting to be embraced by people who call themselves designers.
What a wonderful
time to be learning and working!
Prototypes and probes: Where do they come from? What do they look like?
Well back to the
story. You asked where the prototypes come from, and what they might look like.
Where they come
from is conversations, same as anything else. And that, by the way, has been a
blind spot of design practice. We’ve spent decades on how to have good
conversations about new ideas, but little attention on the conversations before that: who needs to be involved,
who’s being left out, what’s going on, what’s possible, what gifts are
available to this situation, what great intention – bigger than ourselves and
our organization – are we aligned toward, what stories are we aiming to bring
to life in the world, how can we hold on to that intention throughout the
process, what are we afraid of, what is driving us (fear? self-interest?
creative fire?), and so on.
It’s one thing to
miss these conversations when you’re making a new blender or hospital
admittance form or whatever. It’s quite another when you’re pursuing the
question we’re talking about, which is basically about the way an organization
can be a place for soulful, life-giving creative participation of the people
who work there. This doesn’t need to feel like church. It just needs to be
open, honest, and big enough. I’m hurrying through this point because it is a
deep well and probably another conversation to have.
So maybe in our
story we get to a place where we have a gathering of people with some
commitment to shift the status quo. They have different ways of going about it,
they’re in different parts and levels of the organization, but they are joined
by a sense that a better way is both possible and deeply desired. And they’re
hip to the complexity of the situation, so they decide to work experimentally
at the edges, rather than planning some kind of frontal attack on the center of
the status quo.
The prompts might
be things like:
- “We have a few
stories of socially / environmentally responsible choices and strategies in our
organization. How might we get more stories like those, and fewer of the
opposite stories?”
- “We have
identified pockets where people are already making something happen in their
corner of the organization. How might we support and amplify their efforts? How
might we connect them? How can we encourage the birth of a community of
practice?”
- “We know that
experiences are more enlightening and persuasive than arguments and
presentations. How might we engage influencers and decision-makers in
experiences that invite them to re-examine their old stories and open to the
idea of creating new ones?”
- “We know that
this conversation is taking place in isolated silos and groups of our
organization. How might we scaffold bridges of relationship and conversation
between like-minded leaders, projects, and teams?”
Imagine the
experiments that might come out of such briefs! I feel funny making up
examples, because the real thing would be much more specific to the people and
organization than anything I can invent. But examples help, so maybe…
- Pop-up studios
and labs: a day or a week of cross-functional exploration, or provocative
experiences of possible futures
- A pecha-kucha
event to help people become aware of each other’s efforts
- Learning journeys
/ strategic immersions: getting people out of the office to experience say:
organizations that are further along in the change we seek for ourselves, the
positive and negative impacts our organization has on people and places,
parallel but relevant skills and contexts that can inspire our own strategies
- Any number of
experimental artifacts, roles, or rituals that might make it easier for some
group of people to live out their values in their work rather than setting them
aside in service to status quo habits and pressures.
Sometimes the
point of the experiment is the results you hope it will yield. Much more often,
the point of the experiment is the way conversations will be born and
relatedness will increase. I wouldn’t imagine any of these ideas, even a
pecha-kucha one-off event, to be standalone. There would be attention before
and after to tend the conditions for conversation and relatedness.
If our fictional
gathering of people has the ability and sponsorship to formalize this work,
they can manage these experiments as a portfolio, learning from them all,
stabilizing or feeding the ones that spark attraction to something positive,
and dampening the ones that don’t. All the while encouraging and hosting conversations,
reflections, and new connections.
But even without
that, this sort of local experimentation and conversational fertilizer can’t
help but nurture the conditions for something new to grow. It encourages the
pioneers. It sheds light on what’s working. It is the natural starting point
for a community of practice, and once something like that has formed you are
well on the way to a new dominant paradigm. The storm has formed.
Are designers prepared for the work of social pattern-shifting?
Okay. Having said
all that, I’ll return to your question about designers’ skills: “…Suspending
presuppositions, seeing through other people’s eyes, reflecting and reframing
with others, … — all skills purportedly in the designers’ wheelhouse….”
Some barriers
I’ve taught now
in three graduate design programs, and have been a visitor to two or three
others. And I’ve spent countless hours among practicing designers and design
leaders in organizations and at conferences and so on. I’m going to throw a
blanket statement over all that, with the disclaimer that there are certainly
many hundreds of exceptions to what I’m about to say.
When I think
about all those students and professionals and managers, what qualities come to
mind besides their skills and qualities—their training, imagination, good
heart, care for craft, and so on? Here are some that come to mind for me:
- They believe that
they have the tools to tackle just about anything, from beginning to end.
- They love to be
recognized for their expertise.
- They’ve been
soaking in the idea that the primary home for design sponsorship and the
exercise of design’s power is the world of business. Which is to say, most
designers think in terms of business goals and intentions.
- They’re so used
to working with technology that they tend to assume (often unconsciously) that
it will somehow be part of the “solution” they design.
- They believe that
the best way to work is in strong small teams. Outside the team they see
stakeholders and “users.” Their idea of participatory work is an afternoon
workshop with stakeholders and users.
- They’re in a big
hurry. Grad school, internships, first jobs, agencies, big companies,
non-profits,… all their experience has been intense, aggressive, non-stop. They
don’t like that this compromises what they know to be good practice: taking
time to really immerse and understand, to explore many directions, giving equal
time to divergence and convergence, not rushing to conclusions, evaluating
alternatives, and so on. They don’t like it, but they don’t know how to fight
against it. And in fact many take pride in the fact that they can get to
results quickly.
- They aren’t in the
habit of stepping back to see the connection between their current project and
the long-term greater good, and when they do they are poorly equipped to stand
on its behalf.
All of these make for terrible
conditions in which to work in the way I’m suggesting is necessary for
fostering social shifts: “suspend presuppositions, see through other people’s
eyes, reflect and reframe with others.”
You are right
that these that these are all close to the heart of design. We could go deeply
into each of those things, but I’ll pick just one to harp on: “with others.”
The critical piece: "Together" -- participatory emergence
What most
designers aren’t trained to do, and what most processes don’t include, is
helping everyone who is somehow a stakeholder in the situation create together.
Yes, designers seem to be well-positioned to become equipped for a truly
participatory, systemic, and emergent way of working. In my classroom
experiences the biggest challenge for designers is to let go of their engrained
sense of themselves as expert problem-solvers who will be the source of the
good ideas and the shapers of the resulting forms.
Design practice
is full of hero mentality. It is still colonial, in the sense of “I’m here with
knowledge and skills to make things better for you, people who aren’t like me.”
Design doesn’t trust the people it calls “users” to be full peers in
co-creation.
When it comes to
the social complexity of organizational culture, no single project will suffice. No single design is sufficient. The
challenge will not yield to research and expertise. You cannot
design-and-implement, you can only bring your gifts to your participation in
the process, your citizenship in the future.
There is plenty
of design-and-implement work to do down in the details, and huge help to be
given in service to insight, communication, facilitation, and so on. But
there’s so much work to be done together before
we know what to design. Designers can make themselves ready for that work by
- expanding their
ability to work in complexity and uncertainty,
- learning to bring
their process expertise into communities of peer co-creators,
- learning to
focus more on the conditions from
which new patterns of relationship and behavior arise—the conditions in which a
storm might form—rather than “solutions to problems.”
It starts with ourselves, and experience trumps persuasion
Regarding the
relative power of experiences versus persuasion to open minds, a past tweet by
Dave Gray seems relevant:
Years ago, I spearheaded a project in
which I sent a diverse set of stakeholders — many strongly committed to very
different perspectives of how potential customers of a proposed business
behaved and what they would want— out into people’s homes and workplaces to
find out. Those experiences opened minds dramatically, subsequent workshops and
conversation resolved most remaining differences of opinion, and the
stakeholders asked that all future projects be run in a similar fashion.
However, one individual — the executive leader of the project — did not engage
in those experiences, and the course of the project (i.e., the nature of the
business offering), though signifcantly affected, wasn’t changed as
dramatically as many argued was advisable.
“The biggest difficulty in this work came from
lack of executive involvement. The team had an experience that transformed how
they saw the company’s place in the world, and which led them to a new kind of
strategic direction.
But then the team found itself having to
persuasively communicate unconventional ideas to executives who hadn’t been
through the same experience. They had remained in the same institutional
structure and old everyday conversation, while the team had been shaken into a
new realization by their travels, new friendships, and serious reflection.”
So, it seems that
one cannot always avoid the need to (attempt to) persuade.
Lastly, the act
of gardening takes time, sometimes lots of time, as you have stated. But we are
already experiencing multiple significant social and environmental crises. Do
we have the time that such gardening requires?
Business as usual: unredeemable?
Marc: Oh, I’m glad you
mentioned “significant social and environmental crises.” I read your conversation
with John Kolko in which you made a half-joke about not pontificating. But two
weeks ago I promised a room full of people that I would start speaking up more
often about a couple of things, and given the topic we’re discussing this seems
like just the right time to do so.
There are a few
important topics that we too seldom talk about in design, and unless we get
brave, stop avoiding them, get humble, and begin the long walk into their wide
territory, we are going to continue to do more harm than good.
Two pillars of our dysfunctional status quo
We stand on and
work in a long history of systems that leave people out, that deliberately give
some people advantage at the cost of other people’s disadvantage and suffering.
In the U.S., that dynamic has been predominately based on race. It’s getting
easier all the time to take ourselves to school on this topic. We don’t talk
about it nearly enough. How must our practices change in order to contribute to
an equitable and just society? Can we start experimenting, making commitments,
and telling each other stories about these changes?
We stand on and
work in a long history of systems built on an assumption of growth as the
measure of success, as the engine of business, as an undiscussed given. Growth
in what? Quality of life? Wellness? Peace? No, growth in one thing. Profit. We
say we practice “human-centered design,” but the fundamental metrics of our
business sponsors and the systems that support them will refuse to put humans
at the center unless they believe it will create more profit.
And as Joanna
Macy says, any third-grader can see that growth has limits in a world of
limited resources. But if you say that in a boardroom they think you’re being
silly.
A story big enough for a lifetime
So we shouldn’t
end this conversation about our hypothetical company without getting seriously
big-picture for a moment. I want to make sure I don’t give the impression that
I believe that with the right new approach and methods, it’s otherwise business
as usual. We have been talking about organizational responsibility and change
at the scale of one organization and an effort of a few years. But let’s not
kid ourselves. This is not a one-project, learn-a-few-new-tricks kind of
conversation.
This is a paradigm
question. It reaches deep below the emotional layer, down into the place of
identity, care, and sense of connection. Millions of managers have built their
entire career on the assumptions that these questions invite us to challenge.
That’s scary, that’s disorienting, and it causes many people to get defensive,
to grip tightly to the story in which they’ve finally come to be comfortable,
to feel known and accepted, to feel capable. The dominant paradigm comes with a
library of how-to books. The next paradigm, the one yet to be born, can
currently offer only a few clues amongst uncertainty.
In light of this,
persuasion is a ridiculously inadequate tool. It’s pea-shooter versus glacier. The
move to whatever a sustainable and equitable society will not be a tidy process
of reason and debate. It will be (and already is) a messy, billion-fingered,
organic, emergent process of co-creation. It will involve creating attractive
alternatives that draw people forward much more than it involves “changing” the
participants in the current paradigm to somehow act differently together. In
the process, I expect that most of the institutions and systems in the center
of the current paradigm will come to an end.
Some say this
great transition, this “Great Turning” compares in scale of impact to only
two previous shifts: the agricultural era and the industrial age: each involved
creation of new alternatives, displacement or destruction of old patterns, and
a shift in societal consciousness.
Now THAT is a
story big enough to live into. Unlike all the previous invitations I have
received in my career—to improve home appliances or a web site, to bridge
division between departments, and so on and on—unlike all of those, I find THIS
invitation too thrilling to refuse.
. . . .
Richard: Thank you for the conversation. You knock me out, Marc. I look
forward to many more conversations.
Marc: That’s kind of you to say. Thank you very much for a fun
conversation, and yes I’m sure there will be more.


















